Prevention and early management of skin cancer for people with albinism
— Tanzanie —
BACKGROUND
Since 2015, the Fondation Pierre Fabre has extended its initiatives to targeted dermatology programmes in the tropics. These conditions, which may seem to be common or benign pathologies, are nonetheless stigmatising, potentially serious diseases when left untreated. On the African continent, where the number of dermatologists is largely insufficient (15 per 15 million inhabitants in Mali, two per 18 million in Niger, for example*), the public healthcare needs are very great. Skin diseases are very common in developing countries, making dermatology one of the four main reasons for medical visits to primary health centres.
The Fondation Pierre Fabre has been alerted to the seriousness and extent of albinism-related health problems in Africa by various associations. This genetic disease, characterised by a lack of pigmentation of the skin, hair and eyes, causes extreme sensitivity to sun exposure. The risks of developing skin cancer and skin disorders are extremely high and studies suggest that most people with albinism die from skin cancer between the ages of 30 and 40 (report by I. Ero, independent expert for the United Nations, 2015).
In sub-Saharan Africa, this genetic condition is four to five times more prevalent than in the rest of the world (in part linked to endogamy), with an occurrence of up to one case per 1,500 people in certain regions. The lack of information on the connection between albinism and skin cancer only exacerbates this situation. Still, these dramatic consequences are, to a great degree, preventable: simple means, such as using sunscreen and wearing appropriate clothing, can prevent these cancers.
Lastly, people with albinism experience major challenges in integration due to ancient beliefs assigning them supposedly magical powers. In some countries, including Tanzania, superstitions lead to mutilation, dismemberment, organ harvesting and murder. Since 2007, various organisations have reported hundreds of assaults linked to witchcraft beliefs and practices in more than 25 countries.
Convinced of its ability to take action in this realm, in late 2015, the Fondation Pierre Fabre put out a call for proposals to about thirty associations in Africa to strengthen programmes supporting information, early detection and medical care for people with albinism. The Foundation chose the programme presented by the Standing Voice association in Tanzania, which, over the past three years, has developed a very successful plan called Skin Cancer Prevention in the regions bordering Lake Victoria.
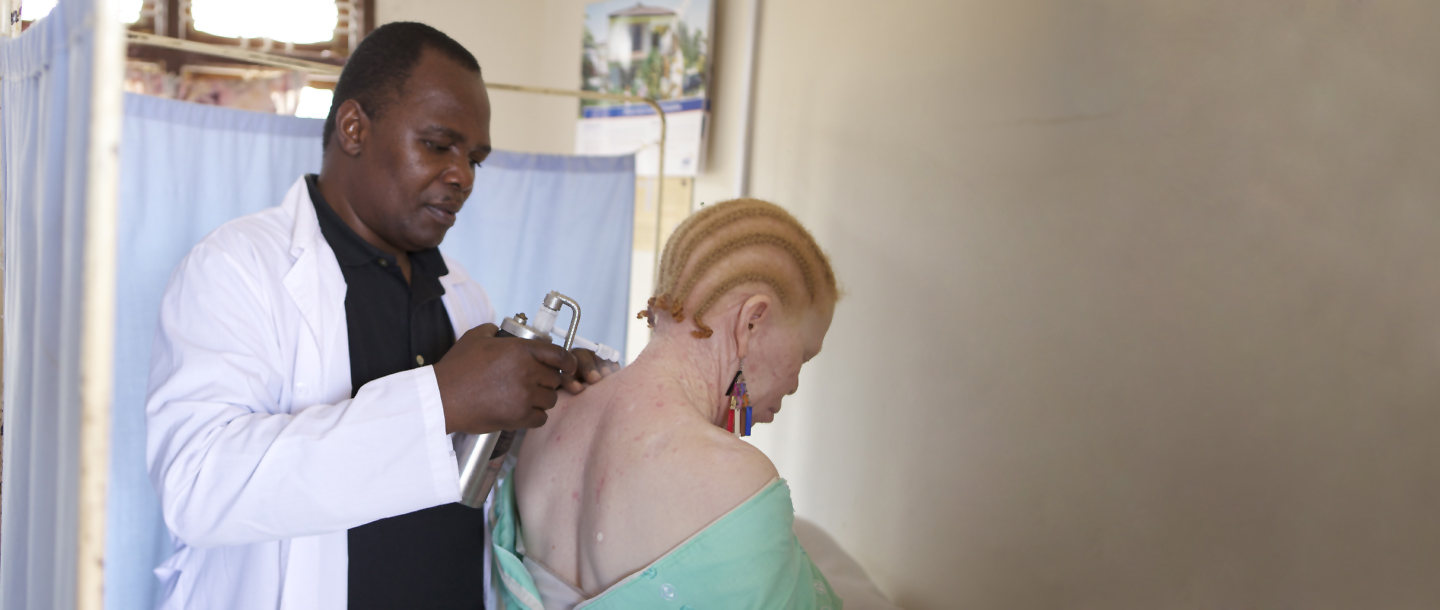
In practice, adults and children (alone or in families) suffering from albinism are invited every four months to “clinics” (medical meetings in specific locations) held in hospitals, schools and “protectorate centers” (rather like orphanages). For one to three days, these people attend dermatologist-led education and awareness sessions. All their questions are answered about the disease, the increased risk of skin cancer and preventive actions to take. At the end of the “clinic”, each person is given a dermatological consultation which, if necessary, gives rise to curative care (for example, treating precancerous lesions using cryotherapy) or referral to a hospital if major surgery is required. More tangibly still, hats and sunglasses are given out at the end of the “clinics”, along with two containers of sunscreen cream, made locally in Moshi at the foot of Kilimanjaro. The two pots provide four months of protection, the period until the next medical visit, and must be returned empty.
Standing Voice oversees 27 scheduled “clinics” every four months in the country, attended by 2,000 people. The first results of this remarkable work were measured concretely by a 71% drop in skin cancer in 465 patients who were monitored over five “clinics” in the Mwanza region.
The Foundation has decided to support this programme for four years by setting the following objectives:
- Developing 16 new “clinics”, in addition to the existing 27, and training eight community dermatologists in prevention and care.
- Developing and supporting training (healthcare workers, community workers and associations)
- Increasing the local sunscreen production capacity to supply another 2,000 recipients, for a total of 4,000 people supplied after four years (with 24,000 pots of cream distributed annually).
- Entering medical data on new patients being monitored into a database and developing clinical research programmes.
- Replicating this “clinic” model to two other sub-Saharan African countries.
*Report by Professor Ousmane Faye, Department of Dermatology, CNAM, Bamako, Mali
KEY FACTS
_____
Priority
Dermatology
Programme
Since 2016
Type of involvement
Distributor
Objectives
- Organise the prevention of skin cancers
- Consolidate patient management by addressing all needs
- Raise awareness among patients, families and communities
THE LATEST PROGRESS
_____
Dermatological treatment
Around 20% new patients every quarter in the 17 regions of Tanzania and 11 districts of Malawi: over 5,900 people treated in Tanzania and 1,600 in Malawi
Ophthalmic treatment
Over 900 patients, mostly children, were examined and prescribed glasses, magnifying glasses or monocular telescopes in Tanzania
Awareness-raising activities
Over 9,300 people attended the awareness-raising sessions and 580 were treated for mental health issues. Creation of support groups and a helpline.
Standing Voice
P.O. Box 180
Nansio
Ukerewe
Mwanza
Tanzania
www.standingvoice.org
Albinism sufferers are one of the most marginalised and vulnerable groups of sub-Saharan Africa, because they are particularly exposed to the risk of skin cancer. Studies estimate that the majority die of skin cancer between the ages of 30 and 40.
Fondation Pierre Fabre is working alongside NGO Standing Voice on the development of special care programmes.This report brings you details of the cancer awareness, prevention and care initiatives rolled out in Tanzania.
Perspectives
Over the next four years, the programme will be consolidated and expanded throughout Tanzania, as well as replicated in other sub-Saharan African countries. By the close of 2020, the objective is to treat 8,000 people with albinism with the support of a team of dermatology specialists providing 24,000 consultations a year. This will have quadrupled the current programme.
PARTNERS
Standing Voice :
Standing Voice is an NGO founded in 2013 that promotes social inclusion and strives to put an end to human-rights violations of marginalised groups. Its founder, photographer and film director Harry Freeland, spent six years in Tanzania producing his documentary In the Shadow of the Sun, aired by the BBC, in which two people with albinism are followed in their daily life, showing their fight against stigmatisation. Standing Voice has a staff of nearly 25 people in Tanzania.
See also
Preventing skin cancers due to albinism
Skin cancer is a major risk for albinos, but the number of dermatologists in Africa is far insufficient. The Foundation takes action.31/07/2025See also
Creation of a national teledermatology service
Mali, faced with a regional dermatologist shortage, is assessing the feasibility of a telemedicine programme. Objectives: improve healthcare and create a true communications network.31/07/2025Follow our actions
An international webinar to launch a major report on the fight against sickle cell disease in French-speaking Africa
On Wednesday 22 April 2026, the Global Coalition Against Sickle Cell Disease organised a webinar dedicated to the official launch of its new report entitled ‘Combating Sickle Cell Disease: Initiatives and Prospects in French-speaking Africa’.




